New research has confirmed long-suspected links between sleep apnea and Alzheimer’s disease, finding identical signs of brain damage in both conditions.
While the cause of Alzheimer’s disease remains a mystery, amyloid plaques that are toxic to brain cells are known indicators of the disease.
The new research by Australian and Icelandic researchers, led by RMIT University and published in the journal Sleep, shows these plaques start in the same place and spread in the same way in the brains of people with obstructive sleep apnoea, as in those with Alzheimer’s.
Lead investigator Professor Stephen Robinson says scientists have known the two diseases are related, but what drives the connection is still unclear.
“We know that if you have sleep apnoea in mid-life, you’re more likely to develop Alzheimer’s when you’re older and if you have Alzheimer’s you are more likely to have sleep apnea than other people your age,” says Professor Robinson.
“The connection is there but untangling the causes and biological mechanisms remains a huge challenge.
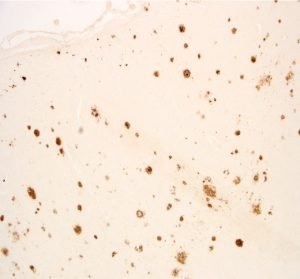
“Our study is the first to find Alzheimer’s-like amyloid plaques in the brains of people with clinically-verified obstructive sleep apnea.
“It’s an important advance in our understanding of the links between these conditions and opens up new directions for researchers striving to develop therapies for treating, and hopefully preventing, Alzheimer’s disease.”
Significantly, the severity of sleep apnea was linked with a corresponding build-up of amyloid plaques.
The study found that treatment with continuous positive airway pressure (CPAP) – the standard approach for moderate to severe sleep apnea – made no difference to the number of plaques found in the brain.
To read the study, visit: academic.oup.com/sleep/advance-article-abstract/doi/10.1093/sleep/zsaa195/5909379?redirectedFrom=fulltext.